What are the 5 components of the Campinha-Bacote model?
The five components of cultural competence
The five components of the Campinha-Bacote model are cultural awareness, cultural knowledge, cultural skill, cultural encounters, and cultural desire. In this model, cultural competence is viewed as an ongoing process of developing these five interrelated components rather than a one-time achievement.
The Campinha-Bacote Model: Five Components Explained
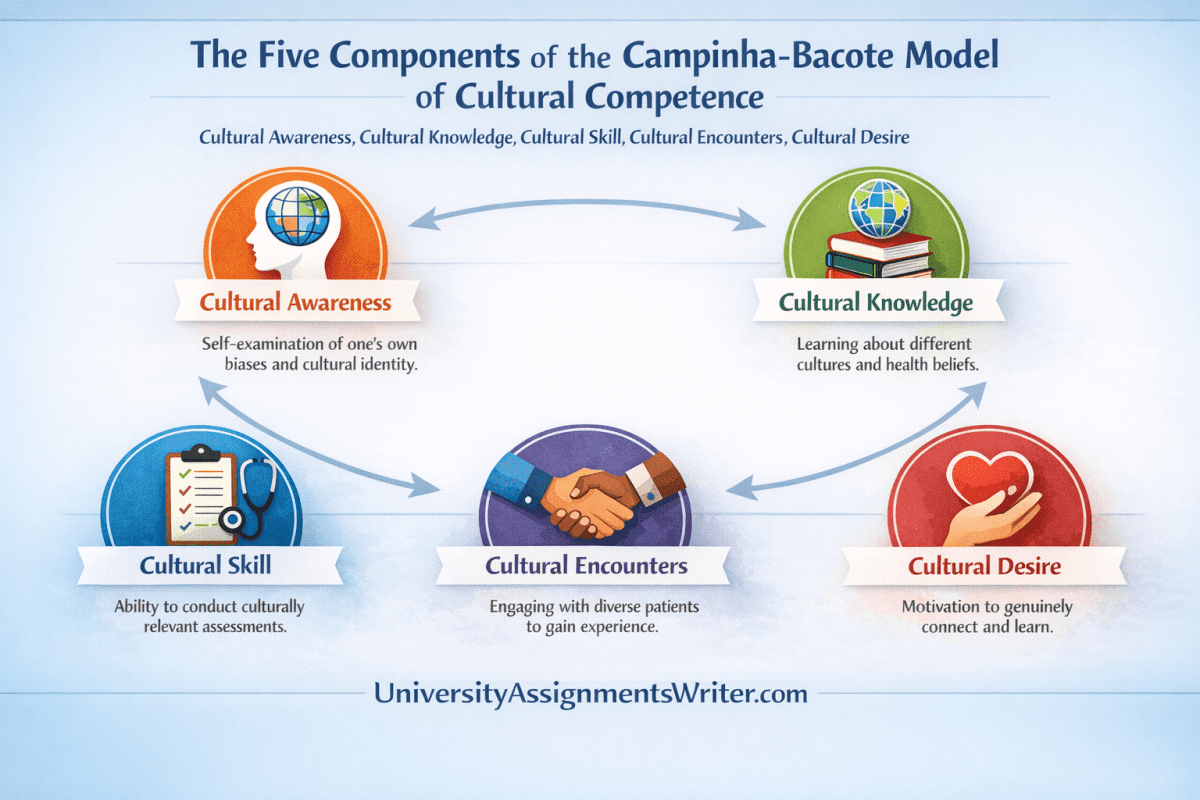
The Campinha-Bacote Model of Cultural Competence in Healthcare (often framed as “The Process of Cultural Competence in the Delivery of Healthcare Services”) emphasizes that culturally competent care is not simply having good intentions or being “respectful.” Instead, it is a continuous professional development process that helps clinicians deliver safer, more effective, and more patient-centered care across diverse cultural identities, values, and lived experiences. The model is widely used in nursing and other health professions because it is practical, skill-based, and grounded in the realities of clinical interaction.
1) Cultural Awareness
Cultural awareness is the deliberate process of examining your own cultural background, values, biases, assumptions, and potential prejudices—and understanding how these can influence clinical judgment and behavior. It includes recognizing the power dynamics that can occur in healthcare (e.g., provider authority, systemic inequities) and how those dynamics may shape patient trust, communication, and engagement.
In practice, cultural awareness shows up when a nurse pauses to ask: “What assumptions am I making about this patient’s choices?” or “How might my own beliefs about family involvement, pain expression, mental health, or end-of-life care influence the way I interpret what I’m seeing?” Awareness also includes acknowledging that “culture” is broader than race/ethnicity; it can include religion, language, gender identity, disability status, immigration experiences, socioeconomic background, and regional norms. Cultural awareness is the foundation because without it, clinicians may unintentionally provide care that is technically correct but emotionally unsafe or misaligned with the patient’s values.
2) Cultural Knowledge
Cultural knowledge refers to seeking and obtaining an educational base about diverse cultural and ethnic groups—especially how cultural factors can influence health beliefs, disease patterns, help-seeking behaviors, and responses to medical interventions. This is not about memorizing stereotypes. Rather, it is learning general patterns while maintaining humility and curiosity, then applying that knowledge carefully to each individual patient.
For example, cultural knowledge helps clinicians understand that some patients may interpret illness through spiritual frameworks, prefer traditional remedies alongside biomedical treatment, or have culturally shaped expectations about modesty, gender-concordant care, or who should receive medical information first (patient vs family). Cultural knowledge also includes learning about social determinants of health and how structural conditions can drive health outcomes—knowledge that helps clinicians avoid blaming patients for barriers like cost, transportation, food insecurity, or limited health literacy. When clinicians build cultural knowledge responsibly, it strengthens communication, education, and shared decision-making.
3) Cultural Skill
Cultural skill is the ability to collect culturally relevant data and perform culturally based assessments in a respectful and clinically useful way. In nursing, this includes interviewing, assessment, documentation, and care planning that reflect the patient’s worldview. It may also involve adapting communication strategies (e.g., using professional interpreters, confirming understanding through teach-back, and avoiding idioms in translated conversations).
Cultural skill can be seen in how a nurse elicits information about pain, diet, family roles, mental health symptoms, and health practices without judgment. For example, a culturally skilled assessment might include questions such as:
- “What do you think is causing your symptoms?”
- “What treatments have you tried so far?”
- “Are there any cultural or spiritual practices you want us to consider in your care?”
- “Who do you want involved in decisions?”
These questions support more accurate assessments and can prevent misinterpretations that lead to inappropriate interventions or poor adherence. Cultural skill also includes recognizing when standard tools (screeners, questionnaires) may not translate well across cultures and adjusting appropriately.
4) Cultural Encounters
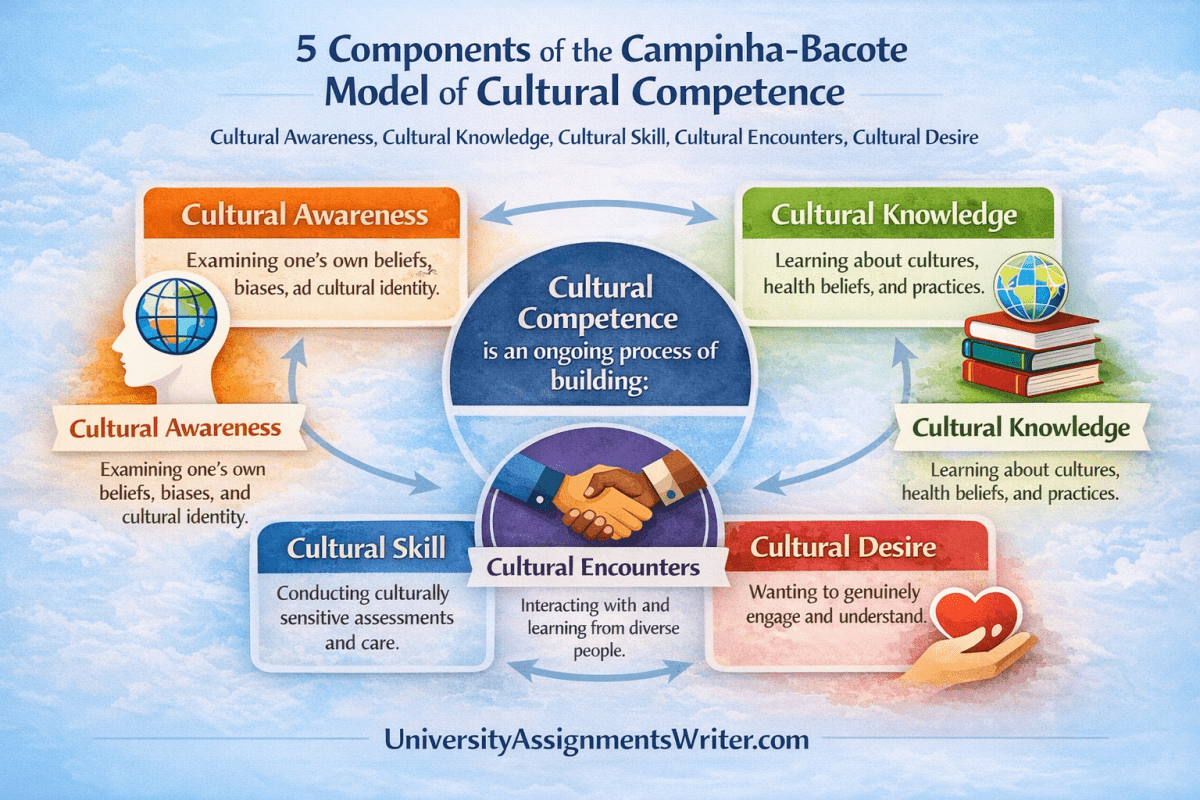
Cultural encounters are the direct interactions with patients and communities from diverse backgrounds that refine or challenge a clinician’s beliefs and prevent reliance on stereotypes. This component is essential because real-world encounters are where cultural competence becomes measurable in behavior—not just in theory.
Through repeated cultural encounters, healthcare professionals learn how culture shows up differently within the same group (e.g., differences shaped by generation, region, education, religion, acculturation, or trauma history). Encounters also build practical confidence: learning how to negotiate care plans when there are differences in beliefs; how to respond when patients decline treatments for cultural or religious reasons; and how to build trust when patients have experienced discrimination in healthcare settings. Importantly, cultural encounters are not “exposure” for its own sake—they should be reflective, respectful, and grounded in professional ethics.
5) Cultural Desire
Cultural desire is the motivation to engage in the process of cultural competence. Campinha-Bacote describes this as the “want to” rather than the “have to.” Cultural desire involves genuine openness, humility, and willingness to learn from patients. Without desire, the other components can become superficial “checklists.”
In practice, cultural desire looks like consistent curiosity and respectful engagement even when time is short, when a situation is unfamiliar, or when biases are triggered. It is also the component most connected to empathy and relationship-centered care. A clinician with cultural desire is more likely to seek feedback, learn from mistakes, advocate for interpreter services, and challenge inequities within systems—not because policy requires it, but because it aligns with professional identity and patient dignity.
How the Five Components Work Together
These five components are not linear steps; they interact continuously. Cultural awareness helps clinicians notice bias and power differences; cultural knowledge provides clinically relevant context; cultural skill supports meaningful assessments and care planning; cultural encounters refine judgment and reduce stereotyping; and cultural desire sustains growth. Together, they support better communication, fewer misunderstandings, stronger patient satisfaction, and improved adherence and outcomes—especially for patients whose experiences differ from the dominant healthcare culture.
References
Campinha-Bacote, J. (2002). The process of cultural competence in the delivery of healthcare services: A model of care. Journal of Transcultural Nursing, 13(3), 181–184. https://doi.org/10.1177/10459602013003003
Campinha-Bacote, J. (2011). Delivering patient-centered care in the midst of a cultural conflict: The role of cultural competence. Online Journal of Issues in Nursing, 16(2), Manuscript 5. https://ojin.nursingworld.org/table-of-contents/volume-16-2011/number-2-may-2011/cultural-competence-and-patient-centered-care/
Saha, S., Beach, M. C., & Cooper, L. A. (2008). Patient centeredness, cultural competence and healthcare quality. Journal of the National Medical Association, 100(11), 1275–1285. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2594253/
Kaihlanen, A.-M., Hietapakka, L., & Heponiemi, T. (2019). Increasing cultural awareness: Qualitative study of nurses’ perceptions about cultural competence training. BMC Nursing, 18, 38. https://bmcnurs.biomedcentral.com/articles/10.1186/s12912-019-0363-x
Kaihlanen, A.-M., Hietapakka, L., & Heponiemi, T. (2019). Increasing cultural awareness: Qualitative study of nurses’ perceptions about cultural competence training. BMC Nursing, 18, 38. https://doi.org/10.1186/s12912-019-0363-x

Dan Palmer is a dedicated academic writing specialist with extensive experience supporting nursing students throughout their educational journey. Understanding the unique challenges faced by nursing students who balance demanding clinical rotations, family responsibilities, and rigorous coursework, Dan provides professional assignment assistance that helps students maintain academic excellence without compromising their other commitments.
With a comprehensive understanding of nursing curriculum requirements and academic standards, Dan delivers high-quality, thoroughly researched assignments that serve as valuable learning resources. His expertise spans various nursing disciplines, including clinical practice, healthcare ethics, patient care management, and evidence-based research.
Dan’s approach combines meticulous attention to detail with a commitment to timely delivery, ensuring that busy nursing students receive the support they need when they need it most. His professional assistance has helped countless nursing students successfully navigate their academic programs while maintaining their professional and personal responsibilities.
Committed to academic integrity and excellence, Dan Palmer continues to be a trusted resource for nursing students seeking reliable, professional assignment support.

